Introduction:
Precise knowledge of the anatomy in some cases is a key for accurate and timely diagnosis. This is particularly true for anatomical variations of development. The bone morphology is a complicated subject since multiple factors play a role in its development and some of them persist throughout life.
Scapula is a flat triangular bone that together with the clavicle and manubrium sternum make up the shoulder girdle. It is a paired bone that is located at the back of the trunk over the ribs two to seven. It provides a point of attachment for several muscles and articulates with the clavicle and humerus therefore forming two important articulations: the glenohumeral and acromioclavicular. The scapula is an extremely mobile bone that allows a wide range of movement for the upper extremity compared to the lower (1). Therefore, dysfunction of the shoulder girdle can significantly affect the daily activities. One of the possible causes of shoulder pain and dysfunction is the suprascapular nerve entrapment by direct nerve compression in the suprascapular notch. The suprascapular notch is the site where the suprascapular nerve and the suprascapular vein, traverses the upper border of the scapula under the superior transverse scapular ligament (2). The suprascapular nerve originates from the upper trunk of the brachial plexus and is a mixed motor and sensory nerve that carries pain fibers from the glenohumeral and acromioclavicular joints and provides motor supply to the supraspinatus and infraspinatus muscles (2). Suprascapular neuropathy was initially described by Andre Thomas in 1936 and leads to pain, weakness of the shoulder with progressive atrophy of the supraspinatus and infraspinatus muscles supplied by the suprascapular nerve (3, 4).
We present a case and review of the literature of an unusual scapular anatomy, where the suprascapular notch coexisted with a foramen. Knowledge of such anatomical variations are particularly important for neurologists, neurosurgeons and traumatologists and should be consider for proper differential diagnosis of patients with shoulder pain and dysfunction.
Case Description
During a routine bone examination, we observed that the left scapula of a 57-year old male cadaver had a suprascapular notch and suprascapular foramen. The length of the superior border, from the base of the coracoid process to the medial angle, was 6.7 cm; the length of the medial border, from the medial angle to the inferior angle, was 12.3. cm; while the lateral border, from the infraglenoid tubercle to the inferior angle of the scapula, was 15.2 cm. The width was 8.4 cm and 6.8 cm in the superior third and the inferior third, respectively. The suprascapular notch had a U shape and the suprascapular foramen was 4x8 mm in diameter (Figures 1 and 2). There were no other anomalies of the scapula.
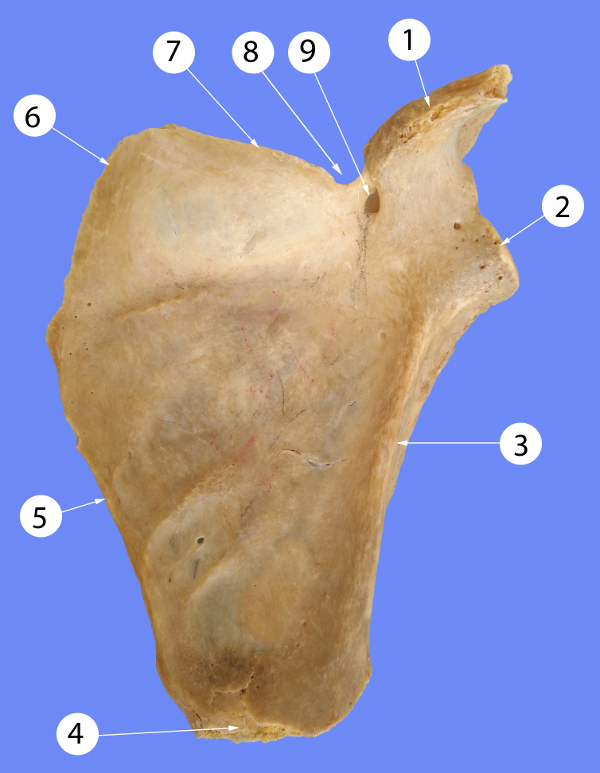 |
Figure 1: Costal surface of the scapula. 1 – coracoid process, 2 – glenoid cavity, 3 – lateral border, 4 – inferior angle, 5 – lateral border, 6 – superior angle, 7 – superior border, 8 – suprascapular notch, 9 – suprascapular foramen. |
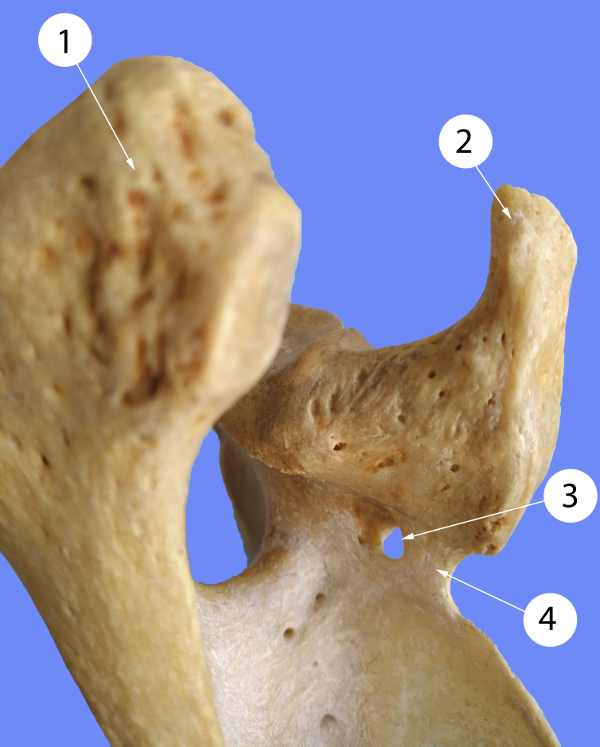 |
Figure 2: Lateral aspect of the scapula. 1 – acromion, 2 – coracoid process, 3 – scapular foramen, 4 – ossified ligament. |
Discussion
The suprascapular notch can be classified into several groups based on the shape of the inferior border of the incisura and a comparison of the vertical and transverse diameters: complete absence of notch (type I, 20% of cases), wide blunted V-shaped notch occupying a third of superior border of scapula (type II, 10% of cases), symmetrical and U-shaped notch with parallel lateral margins (type III, 52% of cases), small V-shaped notch (type IV, 4% of cases), U-shaped notch with partial ossification of medial part of suprascapular ligament (type V, 10% of cases) (5).
Ossification of ligamentous structures during lifetime is a relatively frequent phenomenon in the human body (6). One of the most common causes of suprascapular nerve entrapment is complete ossification of the superior transverse ligament which can be encountered in 1,5-12,5% of cases depending on the region and population (3). Another possibility is ossification of the anterior coracoscapular ligament. Avery and coworkers in 2002 described that in 60% of cases there is a ligament located on the anterior aspect of the suprascapular foramen which was termed the anterior coracoscapular ligament. In 41% of cases it was present bilaterally and was associated with a substantially narrowing the suprascapular foramen (7).
Therefore, suprascapular foramen appears due to ossification of either superior transverse scapula ligament or anterior coracoscapular ligament. In rare cases when both ligaments are ossified this can lead to two suprascapular foramina (8).
The suprascapular foramen can be classified in band and fan-shaped based on its form. The clinical significance is that the band-shaped type is more common and reduces the space below the ligament to a significantly greater degree (9) . In our particular case the foramen was fan-shaped. The coracoscapular ligament can also be classified in fan-shaped (type I), band-shaped (type II), bifid (type III) and vestigial (type IV) (10).
Coexistence of suprascapular notch and foramen is a rare and there have been only a few case reports in the literature (11-14) . This is usually due to ossification of the coracoscapular ligament and intact non-ossified superior transverse scapular ligament. Coexistence of the notch and foramen possibly increases the risk of suprascapular nerve entrapment by nerve irritation of the bony margins during passage through the foramen as this area becomes narrow (13).
The diagnosis of suprascapular nerve entrapment syndrome is typically based on interview, physical examination, and complementary tests such as X-ray, ultrasonography, MRI, and CT. In more difficult cases electromyography and evaluation of the conduction speed from the nerve point of the neck to the supraspinatus and infraspinatus muscles can be performed (3).
Conclusion
Suprascapular foramen is a relatively rare anatomical variation which results due to ossification of superior transverse scapular ligament or anterior coracoscapular ligament. Anomalies and variations of development have special clinical importance and sometimes can be overlooked or misdiagnosed by medical specialists. Suprascapular foramen can lead to suprascapular nerve entrapment syndrome therefore should be considered as a part of differential diagnosis. The coexistence of a foramen and notch is a particularly rare cases and can leads to nerve compression.
References
- Cowan PT, Mudreac A, Varacallo M. Anatomy, Back, Scapula. StatPearls. Treasure Island FL: 2020, StatPearls Publishing LLC.; 2020.
- Zehetgruber H, Noske H, Lang T, Wurnig C. Suprascapular nerve entrapment. A meta-analysis. International Orthopaedics. 2002;26(6):339-43.
- Labetowicz P, Synder M, Wojciechowski M et al. Protective and Predisposing Morphological Factors in Suprascapular Nerve Entrapment Syndrome: A Fundamental Review Based on Recent Observations. BioMed Research International. 2017;2017:4659761.
- Pecina M, Cummins CA, Messer TM, Nuber GW. Who Really First Described and Explained the Suprascapular Nerve Entrapment Syndrome? JBJS. 2001;83(8).
- Kannan U, Kannan NS, Anbalagan J, Rao S. Morphometric study of suprascapular notch in Indian dry scapulae with specific reference to the incidence of completely ossified superior transverse scapular ligament. Journal of Clinical and Diagnostic Research: JCDR. 2014 Mar;8(3):7-10.
- Covantev S, Mazuruc N, Belic O. Kimmerle Anomaly – An Important Anatomical Variation. Online J Health Allied Scs. 2018;17(3):8.
- Avery BW, Pilon FM, Barclay JK. Anterior coracoscapular ligament and suprascapular nerve entrapment. Clinical Anatomy (New York, NY). 2002 Nov;15(6):383-6.
- Covantev S, Belic O, Mazuruc N. Double suprascapular foramen: a rare scapular notch variation. Russian Open Medical Journal 2016;5: e0306.
- Polguj M, Sibinski M, Grzegorzewski A, Waszczykowski M, Majos A, Topol M. Morphological and radiological study of ossified superior transverse scapular ligament as potential risk factor of suprascapular nerve entrapment. Biomed Res Int. 2014;2014:613601.
- Polguj M, Jedrzejewski K, Topol M. Variable morphology of the anterior coracoscapular ligament – A proposal of classification. Annals of Anatomy - Anatomischer Anzeiger. 2013;195(1):77-81.
- Hrdlicka A. The adult scapula. Additional observations and measurements. American Journal of Physical Anthropology. 1942;29(3):363-415.
- Sinkeet SR, Awori KO, Odula PO, Ogeng'o JA, Mwachaka PM. The suprascapular notch: its morphology and distance from the glenoid cavity in a Kenyan population. Folia Morphologica. 2010 Nov;69(4):241-5.
- Polguj M, Jedrzejewski K, Majos A, Topol M. Coexistence of the suprascapular notch and the suprascapular foramen--a rare anatomical variation and a new hypothesis on its formation based on anatomical and radiological studies. Anat Sci Int. 2013;88(3):156-62.
- Natsis K, Totlis T, Tsikaras P, Appell HJ, Skandalakis P, Koebke J. Proposal for classification of the suprascapular notch: a study on 423 dried scapulas. Clinical Anatomy (New York, NY). 2007 Mar;20(2):135-9.
|

