Introduction:
Breast cancer represents about 25% of all cancers in women.(1) In India cancer has become one of the ten leading causes of death.(2) It is estimated that there are nearly 2 to 2.5 million cancer cases at any given point of time in India. Dakshina Kannada, a district of Karnataka state with a population of 2,089,649 as per 2011 census with a density of 430 people per sq.km, released by directorate of census operations in Karnataka.(3) Breast cancer is a disease that instills feeling of dread and fear among many women. It is not only a dreadful disease, but it affects a part of the body that is central to women’s sense of womanliness and feminity also. There is a steady increase in breast cancer incidence among rural women since rural women are increasingly adopting urban lifestyles, reproductive habits and are also increasingly exposed to similar environmental factors as urban women due to economic development.(4)
The emotional impact of cancer diagnosis, symptoms, treatment, and related issues can be severe. Not all breast cancer patients experience their illness in the same manner. Health-related quality of life is now considered an important endpoint in cancer clinical trials. It has been shown that assessing quality of life in cancer patients could contribute to improved treatment and could even be as prognostic as medical factors could be prognostic.(5)
Several studies on prevalence rates have found that one-third of the cancer population experiences distress and may profit from early psychosocial intervention. Between 10% and 50% of cancer patients have been found to have depression, depending on the stage of disease and the methods used to assess depression. Most studies report the prevalence of major depression in cancer patients to be 20% to 25%, increasing with higher levels of physical disability, advanced illness, and pain.(6) The National Comprehensive Cancer Network (NCCN) in 2003 addressed the stigma attached to psychological problems and chose to use the word "distress" because it is more readily accepted and less embarrassing than a psychological or psychiatric term.(7)
Despite a massive amount of research on quality of life after a breast cancer diagnosis, the evidence-based knowledge gap of when, how, in what form, and what the women themselves desire to receive support about, leaves the health care professionals with very limited hands-on guidance for their everyday clinical practice. As such, even though there is some evidence that psychosocial support is helpful, until more solid evidence is available of its effectiveness, humanitarian and ethical values provide the basis and guide for the provision of professional psychosocial support. However, regardless of whether effects on any quality of life measures are detectable or not, psychosocial support and its availability may nevertheless hold a value for those women who desire it.
Methods
Search Strategy
The search was included the literatures published from January 2005 to December 2016. A literature search was done from the data bases such as PubMed, Cochrane Library, CTRI, IndMED and Google scholar. Search terms used were (((("quality of life" OR "psychological distress"))) AND (("family therapy"[Title/Abstract] OR "psychotherapy"[Title/Abstract] OR"cognitive behavioral therapy"[Title/Abstract] "counselling"[Title/Abstract] OR "psycho-education"[Title/Abstract] OR "guided imagery"[Title/Abstract]))) AND (("breast cancer"[Title/Abstract] OR "breast carcinoma"[Title/Abstract] OR "women"[Title/Abstract] OR "females"[Title/Abstract] OR "Breast neoplasm"[Title/Abstract] OR "breast tumor"[Title/Abstract])). We also checked the reference lists of all studies identified by the above methods.
Selection strategy
Randomized controlled trial (RCT) designs, and clinical controlled trials (CCTs) which have made some attempt to address the psychosocial interventions on psychological distress and quality of Life issues among breast cancer cases were selected for the review with women between the age of 18-65 years of a histologically confirmed diagnosis of breast carcinoma of an early non-metastatic stage (Grade I-III) as defined by the TNM (tumor, lymph nodes, metastasis) staging system.
Two stage screening process were done; first stage to screen the articles based on titles or abstracts and second stage screening the full text articles. Titles and abstracts of studies identified during the literature search were screened by two investigators. Potentially eligible studies were read in full by the review author to determine whether or not they meet the eligibility criteria. Any clarifications were discussed with a third author until consensus was reached. Excluded studies were recorded in the 'Characteristics of excluded studies' table. The study selection process was documented in a PRISMA flow chart. Articles which were published in English language only were included.
 |
Fig 1: Study flow diagram (PRISMA) |
Review strategy
Data from all relevant studies were extracted using a pretested extraction sheet and entered into the 'Characteristics of included studies' table in RevMan 5.3 (RevMan). All studies were appraised independently by two review authors. Any disagreement was resolved by discussion. Extracted included the following data:
(a) Participants: country of origin, sample size, setting, diagnostic criteria, age, ethnicity, date of study and data on baseline psychological morbidity for assessment of effect modifiers.
(b) Methods: study design, methods of allocation, allocation sequence concealment, blinding, and exclusion of participants after randomization, proportion and reasons for loss at follow up.
(c) Interventions: type, dose, length and frequency of intervention (for each intervention and comparison group).
(d) Outcomes: type of outcomes, assessment instruments, assessment time point, and follow-up time point.
If mentioned, sources of funding were recorded in the 'Characteristics of included studies'.
For studies with more than one publication, the first publication will be considered as the primary reference but data will be extracted from all of the publications.
The review authors worked in pairs to assess the methodological quality of each selected study covering the area of random allocation, allocation concealment, blinding and loss to follow up. A funnel plot corresponding to the primary outcome was generated to assess the potential for publication bias. Primary outcomes were classified as continuous outcomes and expressed as standardized mean differences (SMD) with 95% confidence intervals (CI) according to the Cochrane Handbook for Systematic Reviews of Interventions, chapter 7, section 7.7.325. All measures of effect included 95% CIs, P values, and for pooled measures the I2 statistic.
Heterogeneity between studies was assessed using the I2 statistic. I2 greater than 50% was considered indicative of heterogeneity. Where marked heterogeneity was suspected, sources were investigated, and where excessive heterogeneity was found estimates were interpreted with caution. Random-effects models were used for all meta-analyses.
Results
Characteristics of selected studies
The search of the electronic databases retrieved 248 publications. After eliminating the duplicates, 233 publications were identified for screening. After this initial screening, the abstract articles were retrieved for the remaining 82 potential studies. From these 62 publications were excluded leaving 20 publications included in the review. Finally six studies were included for the qualitative analysis and from that only four studies were included for the quantitative analysis or meta-analysis.
Only RCTs were included in the review. Therefore, all 6 included studies reported a baseline assessment and a post-intervention assessment. However, the total number of post-intervention assessments varied. The sample size across the 6 included studies varied between 76 and 558, with a total of 1404 participants. The mean number of participants was 234.(8-13)
Characteristics of Intervention
In the context of this review, setting describes the discipline of the intervention administrator and mode of delivery. The most common discipline to administer psychosocial interventions with diagnosed patients was registered nurses, across 3 trials.(10-11,13) A further three interventions in studies were administered by multi-disciplinary teams of social workers, one with Medical breast cancer specialist, Nurses, Social worker, Psychologist and Physiotherapist,(9) one study was exclusively with Social worker and Psychologist(12) and one study with Post -doctoral fellows and advanced pre-doctoral trainees in clinical psychology.(8)
Mode of delivery also varied across studies, with two exclusively face to face education intervention studies,(8,10) two studies with direct face to face interaction with telephonic interaction,(13, 11) one study with direct individual as well as group sessions,(9) and the last one with direct session along with Audio-visual methods.(12)
Characteristics of Participants
Disease characteristics
All the studies (n=6) included only breast cancer patients aged between 18-65 years old. None of them included breast cancer with advanced stage (stage IV).
Interventions
The studies need to be homogeneous to ensure that a combined analysis is valid in order to consider the use of pooled estimates in a systematic review. The effect of a psychosocial intervention is a function of the supportive relationship between the ’trained helper’ and the individual diagnosed with cancer was the basis on which principle we have approached this. The supportive human interaction is present across all trials, as is the common aim to alleviate distress and improve quality of life in the event of a cancer diagnosis. In the current review, features of the selected studies have been considered in this way and, to facilitate careful planning, we have uses a priori definitions and analytic strategies. The subgroups were selected to address the variations across outcome measures, intervention types etc.
Theoretical basis
All the studies included some form of supportive relationship, defined by interpersonal dialogue involving a ’trained helper’ and an individual participant. The theoretical basis within the interventions varied markedly. Some were based on one or two elements, while others used multiple techniques. Three studies considered Psycho-education based intervention,(13,11, 10) and one study was carried out with cognitive therapy and psycho-education,(8) one study with Psycho-education with psychotherapy(9) and the last study was taken Psycho-education with Video and standard print material.(12)
Duration
Out of the 6 studies all the studies reported a specific number of sessions delivered to the intervention group. Amongst those studies the number of sessions varied from one to 10, and some stated the percentage of the intervention group who took part in more than a specified number of sessions. The length of sessions was between 10 and 90 minutes, whereas the frequency of sessions fell between once a week’ and ’once every two months’.
Control intervention
Out of six studies, two studies participants in the control group did not receive the intervention but received standard care and standard information on treatment.(10,9) In one study there was a wait control group,(11) another study there was a usual care with a booklet,(13) one took one day seminar as control group(8) and the last study took different interventions as control for each other.(12)
Outcomes
Four studies provided outcome measure of psychological or emotional distress(8, 9,12,13) and three studies provided outcome measure of Quality of life.(9,11,13) Two studies gave information about depression and anxiety which was considered as part of psychological distress.(10,12)
Excluded studies
Reasons for excluding publications were: a)Studies were not intervention studies, e.g. studies were reviews, or comments; b)Studies evaluated were not psychosocial interventions or were part of alternative and complimentary medicines e.g. guided imagery, hypnosis, yoga or massage; c) Studies were not RCTs, e.g. studies did not have a control group, or participants were not randomized; d) Studies did not focus on Breast cancer patients, or only a part of the sample were Breast cancer patients; e) Studies have outcome measure as other variables which are not under the study e.g: sexual dysfunction or fatigue; f) Study was conducted before the year 2005; g) Study with participants of co-morbid psychiatric conditions, e.g. co-morbid major depression
Methodological Quality
The results of the methodological quality assessment are described in the ’Risk of bias’ tables.
The possibility of bias could be found in the characteristics of the samples. The exclusion criteria varied between the included studies, for example some studies excluded patients with co morbidities, while some studies did not describe any additional exclusion criteria. The methodological quality might also introduce bias. As per the Risk of Bias table there were high risk of 20% in random selection and allocation concealment in the overall studies. Performance bias and detection bias were having more than 75% of unclear bias risk. Attrition, reporting and other bias were having low risk of bias.
 |
Figure 2: Risk of Bias graph |
Effects of interventions
Since the interventions, outcome measures all varied among the studies, the complexity in the data extracted did not allow combining the studies for meta-analysis. However various studies analyzed for its effect on the outcomes of psychological distress and quality of life. The following section provides a description of the results of the meta-analytical examination of the primary outcome QoL and general psychological distress. Also presented is a brief narrative description of the studies that did not present adequate data for meta-analysis.
Psychological distress - Psycho-education Vs No intervention
Both the observation points (6 weeks and 6 months) the interventions proved its effectiveness.(10,12) Two studies contributed for 6 months observation which was found to be effective (SMD - -7.10 95% CI-8.09 -6.10), whereas only one study contributed for 6 weeks analysis,(10) with a strong significance (SMD -5.50 95%CI -6.44 -4.56). However, the percentage variability in effect estimates that was due to heterogeneity rather than sampling error (chance) was high (P < 0.00001, I2 = 81%). The heterogeneity found was likely to reflect differences in size and character of the patient populations examined, possible differences in the contents of the intervention, the mode of delivery or the discipline of the ’trained helper’, as well as differences in the methodological quality of the different trials. However, if that was the case, we might expect heterogeneity to be high across every meta-analysis in the review. The unexplained level of heterogeneity rendered the results inconclusive.
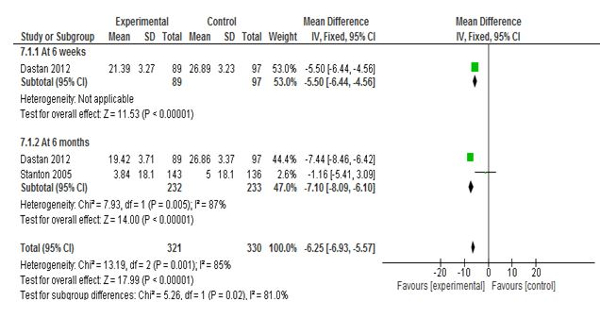 |
Figure 3: Forest plot – effect of Psycho-education on Psychological distress |
Quality of life -Effect of Psycho-education Vs wait control group
Figure 4 shows only one study which was classified as primarily psycho-educational,(11) although a number of others were designed with an educational component. Although it could not prove significant difference may be due to a less well known validated measure of QoL was used, the Meneses et al RCT involved 250 breast cancer participants in an adequately randomized design with no indication of other methodological concerns (SMD 0.02; 95% CI -0.11 to 0.15). Further replication of the results would increase confidence in the conclusions about the value of a psycho-educational intervention across wider groups of cancer patients and cancer sites, particularly if they used more commonly recognized validated measures of QoL to promote more robust comparisons across studies.
 |
Figure 4: Forest plot for Quality of life -Effect of Psycho-education Vs wait control group |
The findings indicate that, to date, there is a lack of convincing evidence to support universal implementation of individual therapeutic psychosocial interventions that are designed to improve the general QoL of newly diagnosed cancer patients. However, the combined effect sizes were small and may not be considered clinically significant. There was notable variation in the style and delivery of psychosocial interventions and the statistically combined results may be susceptible to criticism in terms of the high level heterogeneity. Heterogeneity across the type of intervention, mode of delivery and discipline of ’trained helper’ presented challenges to the review process despite the combined estimates for the outcome measures of psychological distress and QoL indicating no significant statistical heterogeneity. Overall, the results suggested that psychosocial interventions add value to cancer care, though more rigorous research is required.
Participants or population examined
It was not possible to analyze subgroups of patients (for example by gender, age, previous mental health conditions or attitudes towards help seeking) due to the limited detail provided in the trial publications included in the review. Cancer is a condition that generally effects older populations, so age at intervention should be considered in assessments of the impact of interventions. Additionally, those with a history of serious illness or those who are aware of genetic cancer risks have a higher risk of distress after a cancer diagnosis and, therefore, may benefit more from supportive interventions. Individuals who expect psychosocial support to be helpful and who feel that other people in their lives would expect them to use such services are more likely to seek support. Research is required to ascertain the potential impact of attitudes towards help seeking on psychosocial outcomes.
Measurement tools
The current review examines results based on validated measures of QoL and psychological distress (including anxiety, depression and mood measures). No significant effect was observed with generic QoL tools in contrast to the cancer-specific measures, which indicated tentatively that psychosocial interventions improve QoL; and the analysis of secondary outcome measures indicated that psychosocial interventions improve mood. The results may suggest that generic measures of QoL are not sufficiently sensitive to capture change and that future studies and reviews should focus on cancer-specific measures or psychological measures that have been tried and tested with cancer populations.
Inevitably, cancer impacts on an individual’s QoL, both physically and emotionally. Cancer-specific measures of QoL assess the impact of cancer and its treatment and, therefore, are designed to be sensitive to cancer-related changes. Equally when interventions are planned within a population that is effectively free of formal psychiatric morbidity we might not expect measures of clinical anxiety and depression to be as sensitive as measures of mood (which are validated across a healthy population). This problem has been discussed in relevant recent meta-reviews of psychosocial interventions in cancer patients(14, 15) and it is a recognized gap in the cancer care research trial literature. The vast majority of trials measure the impact of a psychosocial intervention on distress in a given population, a proportion of who are not experiencing distress. This approach appears to significantly dilute the treatment effects of psychosocial interventions across trial populations.
Type of interventions
The promising nature of the results examining psycho-educational interventions may be related to the value of knowledge in times of extreme uncertainty. Psycho-educational interventions specifically address emotional concerns arising from the distress that can be caused by being overwhelmed or confused (with, for example, medical terminology, treatment options, side effects, prognosis and how to process and discuss all of the above with loved ones). “Women with breast cancer who are adequately informed about the process experience less psychological distress. However, in many studies, the majority of the women reported needing increased educational support, including written information and the availability of access to a healthcare provider”.(10,11)
A recent study of psychosocial adjustment amongst cancer survivors concluded that despite the increased risk of psychological disturbance in cancer survivors, which paradoxically tends to be more pronounced in younger patients, cancer survivors can also show increased resilience in other domains of psychosocial adjustment thought to be related to post-traumatic growth, such as social wellbeing, spirituality and personal growth. For these reasons, the appropriateness and sensitivity of measures used to assess risk and outcomes form a critical element of any RCT designed to test the effectiveness of psychosocial support for cancer patients.
Conclusion
The review suggests tentatively that nurse-led interventions delivered in person or by telephone could provide valuable improvements in illness-specific QoL and mood, as part of a package of cancer care. However, currently there is not enough evidence to support universal application for all patients. Risk screening is required to identify and target patients who are at most risk of emotional difficulties and, therefore, most in need of support, along with consideration of a range of possible intervention types to suit identified need. The use of tiered intervention approaches in response to strategic periodic risk screening to identify levels of need is recommended in the international guidelines for psycho-oncology. Oncology teams may benefit from considering and assessing the economic and practical viability of formalizing psychosocial support provision as part of the role of specialist cancer nurses within existing health service structures.
Future research directions
A key finding of the review is that existing co-morbidity and risk assessment have not been robustly explored in the RCT context, making this an obvious next step in developing advanced research knowledge about appropriate services that can fulfill the existing guidelines and emerging international psycho-oncology practice guidelines for supporting cancer patients at the time of diagnosis.
Research trials identified for this review targeted patients according to cancer diagnosis alone, rather than primarily considering patients’ perceived need for support. Randomized controlled trials testing psychosocial interventions that are targeted according to need in newly diagnosed cancer patients are lacking. It is necessary to improve the evidence based on need that is, based on what works for people experiencing increased levels of distress. This approach would help to reduce the potential for measurement ’floor effects’, in those who are not experiencing distress, to dilute the observed effects of psychosocial interventions.
The varied quality of reporting has led to difficulties identifying and classifying studies, due to the wide ranging variations in terminology that is used interchangeably in the field of psychosocial support. In the fields of psychological, psychosocial and social care research it is particularly important that publishers remain mindful of the need for authors to provide results according to gender and age, given the documented gender differences seen in accessing psychosocial cancer support and the general lack of gender-specific or age-specific results presented in the trials included in the present review (with the exception of intervention trials carried out with gender-specific cancers such as breast cancer).
The measurement of outcomes is more complex in psychosocial research than in most drug-based studies and clinical measures. However, the increasing number of publications of psychosocial interventions indicates this is an area of huge interest that is gaining increased support from funding bodies. A key feature of the RCT methodology design is the aspect of blinding, but a placebo cannot be effectively administered in trials of psychosocial interventions. Blinding outcome assessors would add to the rigor of the research in this field. Additional insights might be gained by generating synthesized qualitative accounts of the impact of interventions. The development of effective ways to combine mixed qualitative and quantitative data in systematic review terms is in its infancy. Future RCT work in this field should address more specific populations based on need; and provide high quality reporting standards.
Conflict of interest statement: The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Acknowledgements: The authors would like to thank the following people who provided support at various stages of the review process.
- Dr Sanal T.S, Assoc Professor, Dept of Biostatistics, Nitte University, Mangalore
- Dr Richard Kirubakiran, Biostatistician, South Asian Cochrane center, Christian medical college-vellore.
References
- American Cancer Society: Breast Cnacer factes and figures 2017-18 Available at https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/breast-cancer-facts-and-figures/breast-cancer-facts-and-figures-2017-2018.pdf. Accessed Dec 13th 2018
- Population based cancer registries consolidated report (1990-96) Available from: http://www.icmr.nic.in/ncrp/pbcr.pdf . Accessed on Dec 13th 2018
- National cancer registry programme report (1981-2001) Available from http://www.icmr.nic.in/ncrp/cancer regoverrview.htm . Accessed on Dec 13th 2018
- Dey S, Soliman AS, Hablas A, et al. Urban–rural differences in breast cancer incidence in Egypt (1999–2006). The Breast. 2010 Oct 1;19(5):417-23.
- Ferrell BR, Grant M, Funk B, et al. Quality of life in breast cancer: Part I Physical and social well-being. Cancer Nursing. 1997 Dec 1;20(6):398-408.
- National Institutes of Health. Symptom management in cancer: pain, depression and fatigue: National Institutes of Health State-of-the-Science conference statement. 2002. Available at http://consensus.nih.gov/2002/2002CancerPainDepressionFatiguesos022html.htm
- Holland JC. An international perspective on the development of psychosocial oncology: overcoming cultural and attitudinal barriers to improve psychosocial care. In Psycho-Oncology 2003 Jun 1 (Vol. 12, No. 4, pp. S267-S267). The Atrium, Southern Gate, Chichester Po19 8sq, W Sussex, England: John Wiley & Sons Ltd.
- Antoni MH, Wimberly SR, Lechner SC, et al. Reduction of cancer-specific thought intrusions and anxiety symptoms with a stress management intervention among women undergoing treatment for breast cancer. American Journal of Psychiatry. 2006 Oct;163(10):1791-7.
- Boesen EH, Karlsen R, Christensen J, et al. Psychosocial group intervention for patients with primary breast cancer: a randomised trial. European Journal of Cancer. 2011 Jun 1;47(9):1363-72.
- Dastan NB, Buzlu S. Psychoeducation intervention to improve adjustment to cancer among Turkish stage I-II breast cancer patients: a randomized controlled trial. Asian Pacific Journal of Cancer Prevention. 2012;13(10):5313-8.
- Meneses KD, McNees P, Loerzel VW, Su X, Zhang Y, Hassey LA. Transition from treatment to survivorship: effects of a psychoeducational intervention on quality of life in breast cancer survivors. Oncol Nurs Forum. 2007 Sep;34(5):1007-16.
- Stanton AL, Ganz PA, Kwan L, et al. Outcomes from the Moving Beyond Cancer psychoeducational, randomized, controlled trial with breast cancer patients. Journal of Clinical Oncology. 2005 Sep 1;23(25):6009-18.
- Yates P, Aranda S, Hargraves M, et al. Randomized controlled trial of an educational intervention for managing fatigue in women receiving adjuvant chemotherapy for early-stage breast cancer. Journal of Clinical Oncology. 2005 Sep 1;23(25):6027-36.
- Jacobsen PB, Jim HS. Psychosocial interventions for anxiety and depression in adult cancer patients: achievements and challenges. CA: A Cancer Journal for Clinicians. 2008 Jul;58(4):214-30.
- Linden W, Grigis A. Psychological treatment outcomes for cancer patients: what do meta-analyses tell us about distress reduction?. Psycho-Oncology 2012;21:343-50.
|

