Introduction:
Chondromyxoid fibroma (CMF) is a rare benign cartilaginous tumour. CMF is accountable for less than 2% of benign tumour of bone and less than 0.5% of bone tumours. It is characterised by a composition of chondroid, myxoid and fibrous tissue. It involves metaphysis of long bones and proximal tibia is the most common location. Patients belong to age group of 10-30 years and more common in males than females [1].
CMF is diagnosed based on its histological appearance of lobulated pattern with stellate cells in chondroid or myxoid background. Small bones of feet are five times more involved than the small bones of hand [2]. Bones of lower extremities are more commonly involved and toes account for 5% cases [1,3].
Recurrences have been noted after surgery [2]. Large lesions may be aggressive locally and recurrence is seen mostly in young patients. This tumour has got malignant potential but there are no cases with malignant transformation reported [4]. Adequate treatment of the lesion can control the recurrence rate [5].
Recurrences are due to incomplete removal, cortical breach by locally aggressive lesion and high mitotic index [6]. CMF of foot and phalanx treated initially with only curettage, curettage and bone grafting should be closely followed up to look for recurrence.
Case Report
A 24 year old male came with history of pain and swelling of left great toe 8 years back. He was diagnosed to have CMF after biopsy and was treated with curettage and fibular bone grafting. The surgery was done in other hospital and old X-rays were not retrievable. He presented again with pain and swelling in the same toe 6 years later.
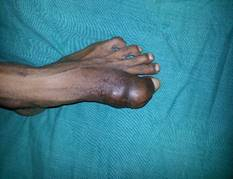
Swelling involved the entire great toe with irregular margins. Skin was brownish black with Scar of 5 cms over the antero-medial aspect of the great toe healed by primary intention. Swelling extended from midshaft of metatarsal to distal phalanx. It was tender to touch with irregular surface and edges indistinct. Range of motion was restricted in MTP and Interphalangeal joint of great toe with sensation being normal (Fig 1).
 |
 |
 |
Figure 1: Clinical pictures of the tumour |
| |

|
Figure 2: X-ray showing the lesion |
Patient was thoroughly investigated with X-ray and MRI. On X-ray, the lesion was expansile, lytic, radiolucent and medullary. The cortex was thinned out with involvement of soft tissues (Fig 2).
MRI suggested of lobulated lesion in proximal phalanx with predominantly soft tissue component. Biopsy was done from the site of lesion and was confirmed to be Chondromyxoid fibroma (local recurrence). No mitotic figures were seen. Under spinal anesthesia, toe amputation was done. Margins were negative and at 2 years follow up, no local recurrence was seen and patient was free of symptoms (Fig 3).
Discussion
Medullary tumours of toe phalanges are rare and among benign tumours, enchondroma are most common. They are radiologically and clinically identical to CMF, hence diagnosis depends on histological appearance [7].
CMF is diagnosed on histopathology as it is composed of myxoid pattern and has osteoclastic giant cells whereas the enchondroma shows cartilaginous tumour with no giant cells [7].
Other benign lesions that involve toes are giant cell tumour and aneurysmal bone cyst which are distinguished histologically from CMF [7].
Malignant tumours like chondrosarcoma are indistinguishable from CMF histologically but aggressive behaviour of tumour is seen on X-ray unlike CMF. Toe is also uncommon area for chondrosarcoma [7].
Various methods of treating CMF are curettage only, curettage and bone grafting, en bloc excision or toe amputation. Curettage plus bone grafting or en bloc excision is suggested to decrease the recurrence [1,2].
A retrospective series of 278 patients showed 11% recurrence after surgery [2]. O’Connor et al. reported 75 % recurrence rate of CMF of forefoot, one of the patient had recurrence 19 years after surgery [9]. There is documentation of malignant potential in the literature [9,10]. Curettage alone [11,12] and curettage with bone grafting [12] showed high rate of local recurrence.
In this case, despite curettage & bone grafting for CMF of great toe, local recurrence was seen. Since there was excessive soft tissue involvement and the toe was not salvageable, amputation was considered.
References
- Schajowicz F, Gallardo H. Chondromyxoid fibroma (fibromyxoid chondroma) of bone: a clinicopathological study of thirty-two cases. J Bone Joint Surg Br 1971;53:198–216.
- Wu CT, Inwards CY, O’Laughlin S, Rock MG, Beabout JW, Unni KK. Chondromyxoid fibroma of bone: a clinicopathologic review of 278 cases. Hum Pathol 1998;29:438–446.
- Fletcher CDM, Unni KK, Mertens F (eds). Pathology and Genetics of Tumours of Soft Tissue and Bone, WHO Classification of Tumours, IARC Press, Lyon: 2002. PP 243 - 245.
- Jaffe HL, Lichtenstein L. Chondromyxoid fibroma of bone: a distinctive benign tumor likely to be mistaken especially for chondrosarcoma. Arch Pathol 1948;45:541.
- Rahimi A, Beabout JW, Ivins JC, Dahlin DC. Chondromyxoid fibroma: A clinicopathologic study of 76 cases. Cancer 1972;30:726-736.
- Sharma H, Jane MJ, Reid R. Chondromyxoid fibroma of the foot and ankle: 40 years’ Scottish bone tumour registry experience. Int Orthop. 2006;30:205-9.
- Wang BY, Eisler J, Springfield D, Klein MJ. Intraosseous Epidermoid Inclusion Cyst in a Great Toe. A Case Report and Review of the Literature. Arch Pathol Lab Med. 2003;27(7):298-300.
- O’Connor PJ, Gibbon WW, Hardy G, Butt WP. Chondromyxoid fibroma of the foot. Skeletal Radiol 1996;25:143–148.
- Bernd L, Ewerbeck V, Mau H, Cotta H. Characteristics of chondromyxoid fibroma: are malignant courses possible? Presentation of personal cases and review of the literature. Unfallchirurg 1994;97:332–335.
- Grotepass FW, Wyma G, Nortje CJ, Farman AG. Chondrosarcoma initially diagnosed as a chondromyxoid fibroma: malignant transformation? Dentomaxillofac Radiol 1988;17:139–143.
- Zillmer DA, Dorfman HD () Chondromyxoid fibroma of bone: thirty-six cases with clinicopathologic correlation. Hum Pathol 1989;20:952-964.
- Lersundi A, Mankin HJ, Mourikis A, Hornicek FJ. Chondromyxoid fibroma: a rarely encountered and puzzling tumor. Clin Orthop Relat Res. 2005;439:171-5.
|

