Introduction:
Haemangiomas are the most common soft tissue tumours of infancy. Despite the
frequency of these tumours, their pathogenesis is not completely understood.[1] Of all haemangiomas of
the body, 0.8% occur in muscles.[2] Intramuscular haemangiomas are non-metastasizing benign hamartomatous
congenital neoplasms, that after remaining unrecognized for long periods, may suddenly start to grow in the
second and third decades of life.[3] These deserve attention not only because of their rarity but also because
of their invariably confusing clinical presentation as well as intriguing etio-pathogenesis.
Case Report
The 14-year-old girl presented with painless swelling on her left forearm
associated with flexion deformity of ring finger. According to her medical history swelling was insidious on
onset and is slowly growing for the past one year. There was history of gradual increase in the flexion
deformity of the ring finger (Fig.1A). For the last two weeks swelling was painful.
On examination the tender swelling was present on anteromedial aspect of proximal forearm with no local signs of
inflammation. Skin over the swelling was pinch able and clinically found to be intramuscular. The swelling was non
compressible and trans -illumination negative. There were no clinical signs of involvement of ulnar neurovascular bundle.
On looking for the transverse mobility of the swelling in the forearm there was associated passive transmitted movements of
the ring finger. The patient was unable to fully extend the finger and passive range of extension of ring finger was more with
the wrist in flexion and ulnar deviation (Fig.1B) suggestive of fixed musculo-tendinous length (Volkmann’s sign positive).
Routine blood and radiological investigations were inconclusive
MRI scan was suggestive of focal haemangioma (Fig.1C)
With appropriate counselling the lesion was surgically explored under timed wakeup anaesthesia in hand[4], which allows us
to confirm appropriate release with complete and total active movements of the digits intra-operatively.
 |
| Fig 1: Isolated flexion
deformity involving ring finger at PIP joint (1A). The
deformity partially corrected on flexion and ulnar deviation
of the wrist joint (positive Volkmann sign) (1 B). MRI
picture of focal haemangioma of proximal forearm extending
from deep fascia into intermuscular plane of flexor muscles
(1 C). |
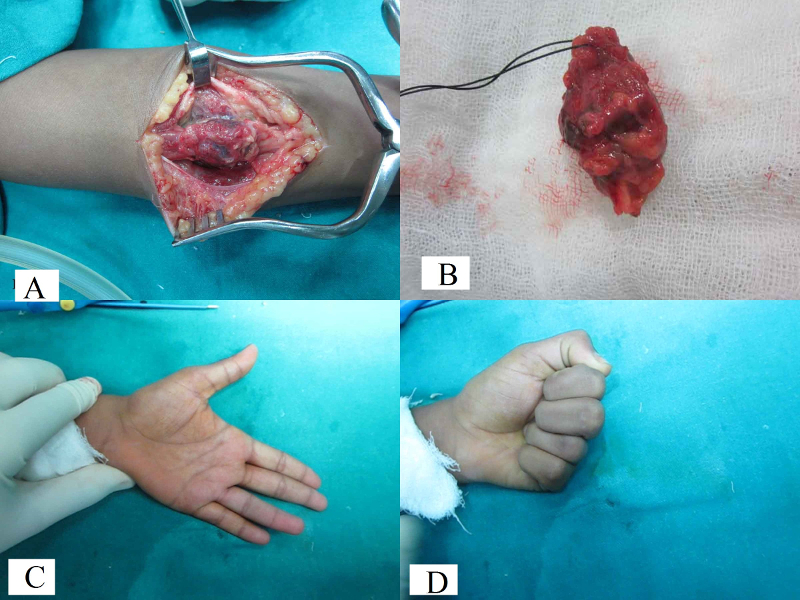 |
| Fig 2: Intraoperative
picture showing the haemangioma involving the FDS of the
ring finger (2 A). Total excision of the swelling including
a normal cuff of the FDS tendon of ring finger (2 B).
Intraoperative complete correction of deformity with full
extension and flexion at PIP and DIP joints (2 C, D). |
Once the tumour was excised in total and the distal end of
Flexor Digitorum Superficialis (FDS) of ring finger was anastomosed with FDS of the middle finger
in an end to side fashion, the tourniquet was released and haemostasis was achieved. Propofol drip was stopped temporarily
2- 3 minutes before the surgeon wanted the patient to cooperate fully for intraoperative active movements. Surgery revealed a
multiloculated purple-red mass arising from musculo-tendinous junction of FDS of ring finger
(Fig.2A). Further, the mass had invaded into the substance of FDS of ring finger with close approximation to neurovascular
bundle. The lesion was excised including the portion of FDS (Fig.2 B). The distal portion of FDS of ring finger was attached
to FDS of middle finger. Complete deformity correction can be assured only if the patient actively flex and extend on table
which is possible only with wide awake surgery. We ensured that the patient was able to fully extend and flex all the fingers
at both MP& IP joints intraoperatively (Fig 2 C,D). This not only confirmed the adequacy of the release but also suggested
that the end to side repair of the ring finger FDS to the mid finger FDS was strong enough for early active controlled
mobilisation of the digits Post excision, the remaining long flexor tendons were found to be uninvolved. The lesion was sent
for excision biopsy.
Histopathological examination confirmed the diagnosis as cavernous haemangioma.
Complete correction of deformity was observed with full extension and flexion post operatively.
Discussion
The life cycle of a haemangioma differs from that of most tumours in that a haemangioma has a
phase of rapid proliferation that is followed by spontaneous involution. Usually arising during childhood, it may continue to
extend either continuously or intermittently throughout adult life.
Every report of the intra-muscular haemangioma in literature stresses its atypical clinical presentation. It is usually
seen as a slow growing mass that may or may not be painful. Features characteristic of vascular tumours like pulsation,
thrill or bruit are generally absent and hence, the condition is rarely diagnosed pre-operatively.[5]
Spontaneous resolution has not been known to occur. Radiotherapy, cryotherapy and embolization have been found to be
largely ineffective. Total excision, often requiring en block resection of the tumour along with the involved muscle is the
universally recommended treatment and was the method employed in the current case.
Various complications have been reported in intramuscular haemangioma, but there is paucity of the literature on
intramuscular haemangioma leading to deformity of digits. Case we are describing is unique by the fact that it has involved
only one tendon of the digit. Previously reported intramuscular haemangioma involving forearm have involved group or multiple
tendons. As reported in literature we did managed to treat our patient with en bloc resection and end to side repair of the
involved tendon to the neighbouring uninvolved tendons.
In conclusion we the authors are presenting this case not only because of rarity of intramuscular haemangioma involving FDS
of ring finger with gross deformity but also the way it was managed under timed wakeup anaesthesia in hand, which not only
ensured that the deformity was fully corrected but also helped us to assess the strength of repair intraoperative when
subjected to full active range of movements.
References
- Drolet BA, Esterly NB, Frieden IJ. Hemangiomas in children. N. Engl. J. Med. 1990;341:173–181.
- Sunil TM. Intramuscular Hemangioma Complicated by a Volkmann’s Like Contracture of the Forearm Muscles. Indian Pediatrics. 2004;41:270-273.
- Vakilha M, Farhan F, Samiei F et al. Intramuscular hemangioma of the forearm. J. Radiat. Res. 2003;1(3):175–179.
- Kamath J, Shenoy T, Jayasheelan N, et al. Timed wake-up anaesthesia in hand: A modification to wide awake surgery of hand. Indian J Plast Surg. 2016;49:378-83.
- Allen PW, Enzinger FM. Hemangioma of skeletal muscle. Cancer. 1972;29:8-22.
|

